MAKING END-OF-LIFE DECISIONS
In order to make good decisions, people nearing the end of life and their families need to know what their choices are. Many of the ideas and terms explained here might be new to you but are very common in medical settings and are important for you to know. There are some difficult issues involved in making end-of-life decisions. We will describe some of the medical conditions and the medical treatments that are often used to keep people alive.
Although modern medicine helps many people lead longer and healthier lives, it has limits. Many of us may fear that medical technology could help us to live longer but leave us dependent on others, unable to think or make decisions for ourselves, and in great pain. Simple humane care focused on our individual needs may be better when no cure is possible.
We hope this information will help you think about these issues, come up with questions of your own, and discuss them with loved ones so that you can make good decisions about the type of care that you want for yourself or your loved ones. Once you have talked about your wishes with loved ones and your doctors, we encourage you to complete an advance directive.
This form allows you to document your wishes for end-of-life care and appoint an agent if you cannot speak for yourself. Please share copies with your doctor, loved ones and agent. (downloadable form)
Free copies of an advance directive are available by calling Kōkua Mau at (808) 585-9977. You can also call the Executive Office on Aging 586-0100 or download copies here.
- NOTE: Bolded words are defined at end of this section.
Promoting Better Communication and Shared Decision-Making
Doctors are, of course, the main source for information about medical conditions and treatment choices. Be sure to ask questions if your doctor uses terms you don’t understand. You have the right to ask questions and to expect honest and thoughtful answers. However, many doctors have been trained to give only facts, not guidance and may not be comfortable making recommendations on end-of-life care.
 Some healthcare workers, like nurses, social workers, and chaplains, are often trained to talk with you and your family about your wishes, hopes, and fears at the end of life. They can help explain the choices you have in making end-of-life decisions and can talk about your goals for treatment and care. These include your quality of life, keeping your independence, being free of emotional and physical distress, and treating illness. These people may be the first to see that a change in your treatment and goals is needed.
Some healthcare workers, like nurses, social workers, and chaplains, are often trained to talk with you and your family about your wishes, hopes, and fears at the end of life. They can help explain the choices you have in making end-of-life decisions and can talk about your goals for treatment and care. These include your quality of life, keeping your independence, being free of emotional and physical distress, and treating illness. These people may be the first to see that a change in your treatment and goals is needed.
Last, but not least, family, friends, and spiritual leaders all bring important but different viewpoints to end-of-life decisions.
Talking things over with all these individuals can help you in making hard end-of-life decisions.
Questions
- What is the prognosis for my condition, and what are my choices?
- What will my life be like with aggressive medical treatments, and do I want to live like that?
- How have other people coped with this?
- Who else can I talk to?
- What kind of end-of-life care is available in my community?
- What does dying mean to me and my loved ones?
- What will help me and my loved ones feel at peace?
- How does my family feel about my wishes?
What is Comfort Care?
Kōkua Mau believes that care at the end of life should be compassionate and should help with your emotional and spiritual needs, as well as controlling pain and treating physical problems (such as shortness of breath, constipation or skin problems.)
The goal of comfort care is to give the best quality of life for the person and family during the time of illness, dying, and grieving. Other terms for comfort care that you may have heard are “palliative care,” “hospice care,” or “supportive care.”
For people near the end of life, quality comfort care would offer more help than the medical procedures (such as CPR, tube-feeding, and dialysis). Start Early. If your goal is quality of life, starting comfort care at the beginning of a serious illness can help a person and family more than waiting until the very end.
Questions
- What will comfort care give me?
- Will I still get any medications for pain?
- Will I be able to stay at home?
- How can I get comfort care?
Medical Conditions
Despite medical advances, the goals of medicine – curing disease, restoring health, and relieving symptoms – do not always happen. People with the following conditions may be kept alive for years by machines and measures that extend life, but will never get well. Comfort care may be better:
- Permanent Vegetative State (PVS). PVS is a deep and permanent unconsciousness. People may have open eyes, but they have very little brain activity and are capable only of involuntary and reflex movements. To confirm someone has PVS requires many tests that take several months. Unlike people with other types of coma, persons in PVS will never “wake up” and get better. People in PVS do not feel hunger, thirst, or pain.
- End-Stage Dementia. Dementias such as Alzheimer’s Disease involve a slow and permanent loss of mental abilities, such as talking, making decisions, and thinking. In end-stage dementia, people are completely dependent on others. They become unable to speak, walk, or move, unable to control bowel and bladder functions; they have less appetite and trouble swallowing and eating, and they do not know loved ones.
Questions
- What will comfort care offer in these conditions?
- Would I want life support to extend my life under these conditions?
- Who should I talk to about my wishes?
- What are the benefits and problems of aggressive medical procedures for people with these conditions?
Medical Technologies
Medical technologies that may be used on dying people include:
- Cardiopulmonary resuscitation (CPR)
- Mechanical ventilation
- Dialysis
- Tube-feeding
Each of these methods is described so that you can better understand what they mean. Any of these can be useful in some cases and not in others-it depends on the person’s wishes, the benefits or problems with the procedure, and the person’s medical prognosis.
We urge you to carefully think about whether or not these medical treatments may be right for you or your loved one.
What About The Costs?
Sometimes, people feel embarrassed or guilty talking about costs when they are facing end-of-life decisions. Nevertheless, the financial burdens on a family can be considerable, and “many families of seriously ill patients experience severe caregiving and financial burdens.” (Source: Covinsky K, JAMA 1994; 272:1839.)
“Discussions with families and patients should include disclosure of the costs involved of the therapy to be offered. . .The omission of financial information denies the patient the right to have the information necessary for informed decision-making.” (Source: Lowance D, Am J Kidney Dis 1993; 21:679.)

Sometimes, there are great emotional benefits associated with family caregiving. But the burdens on families also may be great, and often cannot be measured in dollars alone. Even with health insurance, Medicare or Medicaid coverage, indirect costs of caregiving such as staying at home with the patient during extended absences from work or school, or providing transportation to and from medical appointments can have a serious impact.
Important Words to Know
Advance Directive: A set of instructions, usually written, that allows you to specify the kind of treatment you would want if you are ill and unable to speak for yourself. Both the “living will” and a “durable healthcare power of attorney” are advance directives and we suggest people have both. You can also tell your doctor what your wishes are. You may change your advance directives at any time. Only you can change your advance directive.
Aggressive Medical Treatment: A range of treatments which use complex, invasive methods to prolong a person’s life, such as CPR, ventilation, or dialysis. Commonly asked in end of life situations: “Shall we continue aggressive treatments or shall we change to comfort care?”
Airway intubation: Putting a tube through the airway to get oxygen into the person’s lungs.
Cardiac arrest: No effective heartbeat.
Cardiopulmonary Resuscitation (CPR): Efforts to start breathing or heartbeat to a person in cardiac or respiratory arrest. more
Catheter: A semi-permanent tube that is put directly into a vein or artery through the skin.
Comfort care/Palliative care: Compassionate care that gives medical, emotional, and spiritual support. The goal of comfort care is to meet the needs of the dying person by seeing that the person is kept clean, pain is controlled and that illnesses are treated, such as headache, rashes, and constipation.
Diagnosis: Identification of a disease from its signs and symptoms.
Dialysis: Removal of waste, salts, and extra liquid from blood by artificial means when the kidneys fail.
DNAR: “Do Not Attempt Resuscitation”
Durable Healthcare Power of Attorney: Allows you to name an agent to speak for you in medical matters if you cannot speak for yourself either because of illness or an accident. Your agent should know your wishes and agree to follow them. This is one type of an advance directive.
End of life: When death as the natural result of illness or advanced age is expected within a limited period of time (usually six months to a year).
Hospice: Care given to terminally-ill persons and their families by a team of nurses, social workers, and other support staff, working together with a doctor. The hospice team helps with the physical, emotional, and spiritual distress that is often part of the dying process. 90% of hospice care is given at home but is it also available in hospice care facilities and in some assisted living and nursing facilities, and in hospitals.
Intravenous: Going directly into the vein.
Mechanical ventilation: Use of an artificial breathing machine (respirator).
Prognosis: Prediction; the likely outcome or result of a disease or medical condition.
Respiratory arrest: Unable to breathe on one’s own.
Symptom Management: Treating physical problems such as headaches, rashes, constipation, dizziness, weakness, and nausea. In comfort care, this can be done without treating the underlying cause of the sickness. For example symptoms can be managed in a person with cancer without treating the cancer itself.
Terminal condition: An incurable or irreversible disease or condition for which life-sustaining procedures will postpone, but cannot prevent, death.
Tube-feeding: Liquid (Hydration) or food (fluid nutrients or nutrition) administered through a tube that is put into the person’s body. Tube-feeding can be used for either a short or long period of time.
What is CPR?
Cardiopulmonary resuscitation (CPR) is the use of life-saving measures when the person stops breathing. CPR can involve applying strong pressure to the chest and mouth-to-mouth resuscitation to someone who is having a cardiac or respiratory arrest. CPR may also include airway intubation, mechanical ventilation, electric shock (defibrillation), and intravenous (IV) medications.
When cardiac arrest occurs in young or otherwise healthy people, CPR is often life saving. CPR is thought to be useful when the chance of getting better is very good.
CPR is rarely life saving when cardiac arrest is due to old age or serious illness. For older people, especially those with weaker bones from osteoporosis, pressing on the chest can break the bones. This can be very painful and lead to serious problems if the person lives. Many people believe that CPR is not correct for people who have said they do not want it, and for people who are not likely to get better.
 Even when CPR “works” and the person begins breathing again, oxygen-carrying blood must get to the brain within 3-4 minutes to stop permanent brain damage. After 20-30 minutes, survival is very rare and, if the person does live, severe brain damage is likely. For this reason, many doctors believe that after 30 minutes without a positive response, CPR should be stopped.
Even when CPR “works” and the person begins breathing again, oxygen-carrying blood must get to the brain within 3-4 minutes to stop permanent brain damage. After 20-30 minutes, survival is very rare and, if the person does live, severe brain damage is likely. For this reason, many doctors believe that after 30 minutes without a positive response, CPR should be stopped.
In Hawaii, if you do not want CPR at the end of life:
- Discuss your wishes with your doctor and family and document them in your advance directive
- “Do Not Resuscitate” or “DNR” bracelet or necklace: The Department of Health in Hawaii announced that the DNR Bracelet program has been suspended indefinitely. All CCO-DNR issued before the program was suspended will be honored. more
- click here for MORE ABOUT CPR
Mechanical Ventilation

Sometimes people who are revived by CPR must use mechanical ventilation to keep on breathing. When mechanical ventilation is used, a machine called a ventilator (or a respirator) is used to take over breathing for a person who cannot breathe naturally. It is important to understand that a ventilator is not a cure in itself: it can only “buy time” to see if the person can start natural breathing again.
- click here for more ABOUT VENTILATION
What is Long-Term Dialysis?
Kidneys are internal organs that filter and clean our blood. When kidneys fail, waste and excess fluid build up in the blood. The job of the kidneys must be taken over by a technique called “dialysis.” There are two kinds of dialysis:
Hemodialysis: A catheter is put directly into the person’s blood vessels, taking the blood through a kidney machine for each dialys is session. People usually need several hemodialysis sessions each week.
is session. People usually need several hemodialysis sessions each week.
- Peritoneal dialysis: A special fluid is pumped into a space surrounding the person’s stomach and intestines and then removed. It picks up the waste that has been filtered out of the blood through a natural membrane.
Using dialysis can often extend a person’s life. However, problems and infections can occur. Long-term dialysis often must be continued for the rest of the person’s life unless a kidney transplant is performed. Dialysis requires a strong, ongoing commitment from people, their families, doctors, healthcare providers, and support staff. It is not a “cure” for kidney disease; it is only a substitute for normal kidney function.
When kidneys fail because of a terminal condition, dialysis will only prolong the dying process.
Many people believe that short-term dialysis should not be used when significant benefit is very unlikely. They also believe that long-term dialysis should not be used for people in a permanent vegetative state, or with severe, progressive, irreversible brain disease, like Alzheimer’s.
Questions
- Am I likely to need dialysis?
- Would it be long or short term?
- What are its benefits and problems?
CLICK HERE FOR MORE ABOUT DIALYSIS
What is Tube-Feeding?
Tube-feeding is a way of giving liquid and nutrients to people who cannot eat 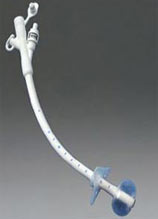 or drink by mouth. Usually, for short-term tube-feeding a lengthy tube (called a nasogastric, or “NG” tube) is put through the person’s nose and esophagus into the stomach. For long-term tube-feeding, a tube may be put directly through the skin into the stomach (called a gastric, or “G,” tube) or the intestines (called a jejunal, or “J,” tube.)
or drink by mouth. Usually, for short-term tube-feeding a lengthy tube (called a nasogastric, or “NG” tube) is put through the person’s nose and esophagus into the stomach. For long-term tube-feeding, a tube may be put directly through the skin into the stomach (called a gastric, or “G,” tube) or the intestines (called a jejunal, or “J,” tube.)
Another form of long-term artificial feeding is “total parenteral nutrition” (TPN). Liquid nutrients are given through a small plastic tube (catheter) that goes directly into a large vein near the person’s heart.
Using tube-feeding can often extend a person’s life. However, some of these techniques can be very uncomfortable and may increase the risk of infection and other problems.
Short-term tube-feeding can help a person through recovery after surgery and severe injury or illness. Many people believe that long-term tube-feeding may be appropriate for people who can still recognize or communicate with others but should not be used for people in a permanent vegetative state or with severe, progressive, irreversible brain disease.
*Information on this page was created by and obtained with permission from the Colorado Collective for Medical Decisions, Inc. (CCMD), 1999, and Hospital Shared Services of Colorado.

